How to find the next pandemic virus before it finds us
Scientists investigate animals for germs that could spill over into people
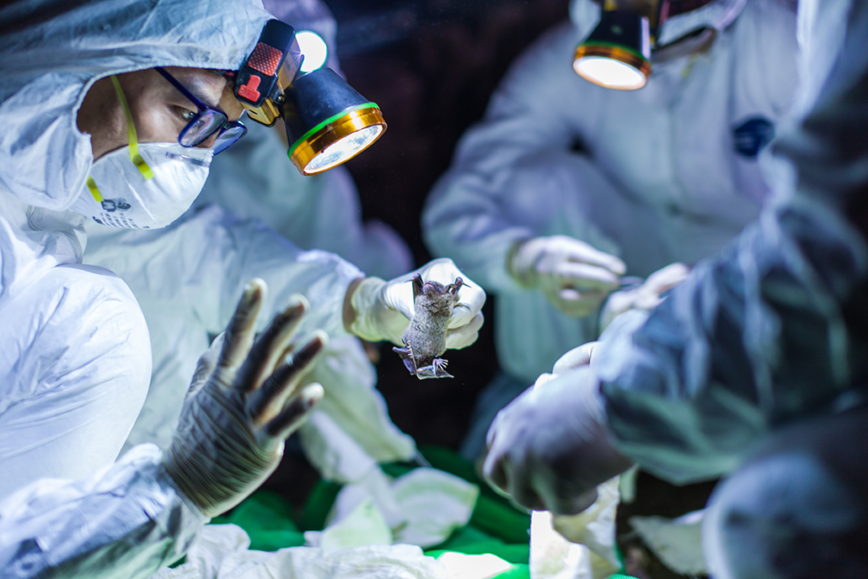
Researchers with EcoHealth Alliance in China remove a bat from a live trap. They will sample blood and feces before freeing the animal. They must wear protective gear in case the bat hosts a harmful coronavirus. They’re scouting for novel viruses that might be able to trigger a pandemic.
EcoHealth Alliance
More than 100 years ago, a deadly flu virus circled the globe. It caused the influenza pandemic of 1918-1919. Before it was over, this disease had sickened an estimated 500 million people. That was one-third of everyone alive at that time. Some 20 million to 50 million people died.
Flash forward to the 1970s. People in a small Central Africa village fell ill with a mystery disease. It caused bleeding that would not stop. Soon, this Ebola virus would spread to other villages.
What do these famous viral outbreaks have in common with the new coronavirus disease known as COVID-19? Scientists believe animals initially carried the viruses that cause all three. Such diseases are known as zoonoses (ZOH-wuh-NO-sees). That means they started in animals and later spread to people.
Flu likely came from birds. Researchers think that bats may have been the source of the Ebola virus and of COVID-19. “Roughly 75 percent of global pandemics and disease outbreaks caused by new viruses come from wild animals,” says Tracey Goldstein. She’s a virus detective at the University of California, Davis. She hunts for new viruses among the wild animals of Africa.
When viruses pass from wildlife to people, it’s called a spillover. Fortunately, spillovers that affect more than a handful of people are rare. But big spillovers do seem to be happening more often, Goldstein and others observe.
To prevent the next big outbreak, researchers around the world are scouting the role of wild animals in the emergence of new human diseases. Scientists want to understand which groups of animals or viruses pose the biggest risks. What they learn could help us all.
Virus hunters turn to bats
Viruses are tiny, infectious particles. They “live” but aren’t technically alive. They can reproduce only within the cells of a living host. That host can be an animal, plant, bacterium or fungus.
“Humans carry lots of viruses,” notes biologist Kevin Olival. He works for a group called the EcoHealth Alliance. Based in New York City, it tries to protect people and wildlife from new diseases. Measles and common skin warts are examples of viral diseases. But not all viruses are harmful, Olival notes. Some seem to have no effect on the body. It all depends on the virus and the host.
“All mammals carry viruses,” Olival says. “But there’s something about bats that might be a little different or unique.” That’s why he has made bats — and the viruses they carry — a focus of his research.
Bats are thought to be the host for a number of relatively new viruses that can sicken people. Among them are the Ebola virus, Marburg virus, Nipah virus and SARS-CoV-2. That last one is the coronavirus responsible for COVID-19. In 2002, another coronavirus from bats caused a massive outbreak of SARS (severe acute respiratory syndrome) in China. Highly contagious, SARS showed some similarities to COVID-19.
Olival and his colleagues at EcoHealth Alliance have been studying the coronaviruses hosted by bats. In China alone, they found 400 different strains of these viruses. Most of them probably wouldn’t sicken people, he says. To figure out which can, researchers will have to perform tests. That will involve taking human cells and infecting them with each virus in the lab, he explains.
Or, researchers could survey people living near the bats and sample their blood. Olival’s colleagues at EcoHealth Alliance were part of a research team that did just that. They worked in rural Chinese villages. And there they found signs that mini coronavirus spillovers have been underway.
The researchers surveyed 1,585 people. They collected blood from 1,497 of them. Of these, 265 (almost one in every six people) reported some symptoms in the past year of a SARS- or flu-like disease. Nine people also tested positive for SARS-like coronaviruses that had previously been found in area bats. None of these nine remembered having any interactions with bats. However, the people who had reported SARS-like or other severe respiratory infections did say they had been exposed to wildlife and livestock.
This suggests that there may be zoonotic illness in these populations. And, the researchers add, the novel bat-linked viruses in the blood of some of these villagers offers “evidence for bat-borne coronavirus transmission to people.” Hongying Li of the EcoHealth Alliance and her colleagues reported their findings in the September 2019 Biosafety and Health.
Educators and Parents, Sign Up for The Cheat Sheet
Weekly updates to help you use Science News Explores in the learning environment
Thank you for signing up!
There was a problem signing you up.
Why bats?
Researchers don’t know precisely why bats are a good host for many deadly viruses. But they have some ideas. Bats are the only mammals that fly. (Other “flying” mammals don’t fly. They only glide.) Flying is hard work. A bat needs about twice as much energy for its flight muscles as a similar-sized rodent needs to run on the ground. Putting all their energy into flying could leave bats with less energy to fight off sickness or injury. But that doesn’t happen. Scientists think that flight may have led bats to evolve stronger immune systems than other mammals.
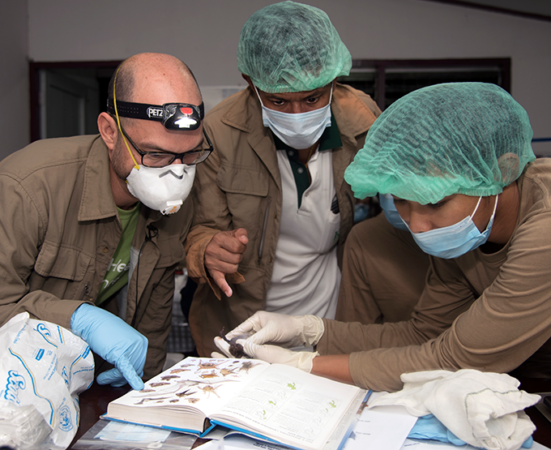
A unique immune system might mean a unique response to viruses. For instance, one recent study showed that bats’ bodies can limit the ability of a virus to trigger dangerous inflammation. That response may push viruses to evolve in ways that let them rapidly spread from cell to cell. And if that altered virus now spreads to a species without such a strong immune system, the new victim might get super-sick — and quickly.
Olival’s work has mainly taken him to Malaysia. This Southeast Asian nation has more than 100 bat species. He wants to better understand how viruses there might spread between different groups of bats. So he collects genetic information from bats and bat viruses. He uses that to build computer models. These computer programs predict which bat viruses could cause real harm in people and other animals, he explains.
Some, such as the Nipah virus, can infect a wide range of animals. Several species of fruit bats in Southeast Asia carry that virus without getting sick. But in 1999, Nipah virus triggered a deadly outbreak among Malaysia’s pigs and pig farmers.
Goldstein’s team performed similar work with bats in Sierra Leone. That’s a country in West Africa. Her group had suspected local bats carried the Ebola virus. It was not a wild guess. In 2014 and 2015, an Ebola outbreak killed nearly 4,000 West Africans. And in January 2015, researchers linked the start of that outbreak to a two-year old boy in Guinea. He liked to play in a hollow tree where insect-eating bats used to live.

Villagers had burned the tree down. But insect-eating bats had been linked to earlier Ebola outbreaks. That made these animals the most likely suspects in the West African outbreak, explained Fabian Leendertz at the time. He works at the Robert Koch Institute in Berlin, Germany. His team described how its detective work led to this conclusion in the January 2015 EMBO Molecular Medicine.
“We wanted to see what other viruses were circulating in bats and other animals” in Sierra Leone, recalls Goldstein. That country shares a border with Guinea. Knowing what viruses the bats hosted might help researchers better understand their viral risks to people.
The bats in Sierra Leone carried Marburg virus, Goldstein’s team discovered. It’s a close relative to the Ebola virus. Marburg causes severe bleeding in people, just as Ebola does. But Marburg has not yet sickened anyone in Sierra Leone. The researchers found the disease in bats before any people got sick. But now Goldstein’s group knows that bats pose a Marburg risk there.
Protecting people and wildlife
Figuring out where potentially dangerous viruses come from is only part of the challenge. Research also needs to identify what activities put people at risk of exposure to animal viruses, note Goldstein and Olival.
These new viral diseases aren’t passing from wild animals to people because animals are going out of their way to mess with us. “It’s because we interfere with them,” says David Quammen. He’s a science journalist. And he researched the topic for a book he wrote eight years ago, Spillover: Animal Infections and the Next Human Pandemic.
Ecology is a branch of biology that explains how different living things interact with each other and their surroundings. And “humans are changing ecology,” observes Hellen Amuguni. She’s a veterinarian and infectious-disease researcher at Tufts University in North Grafton, Mass. People can alter ecology by cutting down trees in forests. Or they might build roads or cities through the landscape. Some might hunt down wild animals for pets or food, explains Amuguni. All of these activities can impact the local ecology in ways that scientists are just beginning to understand.
One new study backs that up. Christine K. Johnson of UC Davis and her colleagues published it April 8 in the Proceedings of the Royal Society B. They found that hunting, wildlife trade, habitat destruction and the spread of cities into areas that were previously wildlands all increase the risk of virus spillovers. Selling wild animals at markets or shrinking their natural habitat can jumble together species that wouldn’t normally meet.

Scientists think that the new coronavirus might have come from a live animal market in China. The virus could have passed directly from a bat to a human. Or it could have passed from a bat to another animal that was touched by a human. Wild animals kept in cages come into close contact with people and other animals. That provides more chances for viruses to spill over from one species to another.
And these events can be just as bad for wildlife as for people, points out Christopher Whittier. He’s a veterinarian at Tufts who studies human diseases that spill over into wildlife. “Understanding what viruses are in wildlife can help us to protect wild animals, too,” he notes.
The human measles virus can sicken and even kill mountain gorillas. Researchers in Africa discovered this back in 1988. People would gather to watch the apes in Rwanda’s national parks. At the time, no one knew that someone’s sneeze can infect local primates with colds and other viral diseases. And there’s plenty of opportunity for that. Each year, park gorillas and chimps were exposed to more people — and their germs — than would visit the average person’s house over a lifetime.
After scientists realized that these wild animals could get sick, practices changed. Today, people visiting wildlife parks in Africa are asked to keep at least 7 meters (23 feet) away from apes to avoid spreading germs.
When you really think about it, human health, animal health and the environment are all connected, says Olival. Preventing the next pandemic will take the work of doctors, veterinarians and scientists. Each field contributes something different to the understanding of new zoonotic diseases. “If we all come together,” he says, “we can improve the health of humans and the planet.”

Editor’s note: This story has been updated with a new image of Olival’s work with bats. It substitutes for an image of work in Gabon.