Cool Jobs: Scents of science
Better understanding of the sense of smell inspires research into everything from whales to electronic ‘noses’

Humpback whales sometimes breach, or leap into the air. Some scientists believe the behavior allows the marine mammals to smell scents wafting over the water.
NOAA
Share this:
- Share via email (Opens in new window) Email
- Share on Facebook (Opens in new window) Facebook
- Share on X (Opens in new window) X
- Share on Pinterest (Opens in new window) Pinterest
- Share on Reddit (Opens in new window) Reddit
- Share to Google Classroom (Opens in new window) Google Classroom
- Print (Opens in new window) Print
By Pippa Wysong
What’s that smell? Your nose probably knows.
Your sense of smell can help you identify a flower by its scent. It can alert you when the milk in the fridge has gone bad. And it can detect the telltale odor of a gas leak. Whatever the task, smell plays a major role in our understanding of the world.
That amazing ability has inspired many scientists to learn even more about how humans and other animals use their sense of smell to find food, detect danger and even communicate. Some have gone on to use that knowledge to improve our health too.
Here, we profile three scientists who focus on smell. They are studying this sense to sniff out exciting discoveries in biology, electronics and medicine. One expert is revealing the unexpected role smell plays in the behavior of whales. Another is developing devices that can sniff scents electronically. And the third is learning how a loss of smell can help diagnose some common diseases.
Leapin’ whales
Much of Julie Hagelin’s work is up in the air. She’s a scientist at the University of Alaska’s Institute of Arctic Biology in Fairbanks. For many years, Hagelin, she has studied the role scents play in wild bird behavior. Then, in 2010, Hagelin heard Jan Straley talk about the behavior of humpback whales. Straley is a marine biologist at the University of Alaska Southeast in Sitka. She mentioned how the huge whales sometimes breach, or briefly leap into the air. But nobody knew why they did this, she added.

The mystery hooked Hagelin. “I always liked watching animals and understanding why they do what they do,” she explains.
So Hagelin asked Straley whether the whales might breach to better sniff the air — maybe to locate food or scout for danger. Straley replied it was an interesting idea. But she added there wasn’t much evidence that humpback whales even had a sense of smell. To investigate the idea further, the two scientists soon teamed up.
In the summer of 2011, Hagelin and Straley set up an observation post in a lighthouse on the coast of southern Alaska. Their post overlooked a region of the Pacific Ocean crossed by humpback whales during their fall migration to Hawaii. The researchers spent hours carefully noting the direction of the giant mammals and of the wind.
“If whales head into the wind, this would be consistent with the idea they could better pick up on chemical scents that the wind blew in their direction,” Hagelin explains.
There was a 1-in-8 chance a whale’s position would coincide with the wind direction, Hagelin explains. Instead, the humpback whales headed into the wind up to half of the time — that is two to four times more often than by chance alone. This didn’t prove the whales breached to sniff odors blown their way, but it suggested it was possible.
Meanwhile, other researchers in Alaska were studying a region of the brain called the olfactory bulb in both humpback and bowhead whales. Olfaction (Oal-FAK-shun) means the ability to smell. Humans, among many other animals, process smells in the olfactory bulb.
In identifying a scent, you might think the nose does all of the work. Instead, its major role is to draw airborne chemicals through the nostrils and pass them across specialized sensing cells. As chemicals come into contact with these cells, they launch electrical signals that travel directly to the olfactory bulb and then elsewhere in the brain for further interpretation.
The researchers discovered the olfactory bulb in the two whale species was more complex than the olfactory bulb found in humans. In the whales, this smell-processing center also took up a share of the brain six times larger than it did in humans.
The brain research, together with Hagelin’s own observations, suggested humpback whales probably can smell just as well as people — and possibly better than. Certainly, a good sense of smell could help humpbacks find the half a ton of krill and small fish that they eat each day, Hagelin notes.
To confirm her hypothesis, Hagelin now plans a new study that will examine whether humpbacks really do use the sense of smell to find food.
Electronic sniffers
What if a machine could sniff out scents too dull, dainty or dangerous for human noses? Such a device could sniff out toxic chemical leaks, ripening crops or even human diseases. In fact, engineers are developing electronic noses to do each of these tasks.
Perena Gouma is an engineer at the State University of New York at Stony Brook. One device that Gouma designed measures tiny traces of chemicals in a person’s breath. Eventually, Gouma hopes the measurements will help to monitor, control or even diagnose different diseases.
One version of the electronic nose could help people with type 1 diabetes. They do not make enough insulin to control the blood sugar released during the digestion of foods. Diabetes patients can inject themselves with extra insulin — but first, they must measure sugar levels in their blood. That means pricking the skin several times a day to draw blood for testing.
“The sugar levels are an indirect way to figure out what insulin levels are like,” Gouma explains. “A small, portable, sniffer device might, some day, replace the need for doing those blood tests.”

This particular sniffer would work by detecting a chemical produced by the body called acetone. Acetone is the same chemical that gives nail polish remover its strong smell. In diabetics, acetone concentrations increase in the breath when insulin levels drop too low. An electronic nose that measures that acetone could alert diabetics when they need more insulin — without drawing blood.
So far, Gouma has built a prototype, or first version, of a handheld acetone sniffer. Patients exhale into a mouthpiece at one end. Inside, a sensor pad coated with special materials reacts whenever it encounters acetone. A small computer chip built into the sensor system measures the size of that reaction and, in turn, how much acetone was present. A digital display then presents that information for a patient to read.
The prototype is now undergoing testing while Gouma refines its design. Eight people exhale into the blocky sniffer several times each day. Four of them have diabetes; the other four do not. Once the study is over, Gouma will compare the results from the two groups, making sure that certain foods or other factors unrelated to insulin don’t affect acetone levels.
Gouma’s team is also working on electronic noses to help diagnose kidney disease and prevent asthma attacks. Asthma is an allergic disease where the airways periodically contract, or tighten. That makes it difficult to breathe. When asthma starts to flare up, levels of a gas called nitric oxide gradually increase in the body. Unfortunately, asthma attacks sometimes build too slowly for patients to notice until the problem becomes severe. So an electronic nose that sniffs out the early signs of an asthma attack could provide a useful warning for these individuals.
“Asthmatics could check their breath a few times a day, and when they spot a rise in nitric oxide they could take medication to prevent an attack before the symptoms become really noticeable,” Gouma says. The kidney disease sniffer would work by analyzing the breath of patients for a chemical called ammonia.
“We are using our science and engineering skills to contribute to improving human health, and that’s very exciting,” Gouma explains.
Sniffing out early brain disease
Sometime pollutants or disease can rob people of their sense of smell, says smell expert Richard Doty. He works at the University of Pennsylvania’s Smell and Taste Center in Philadelphia. There, he leads a team that has studied the problem since the 1980s.
Back then, people knew little about what and how well people could smell. Doctors simply lacked a tool to measure people’s scent detection. So Doty developed a smell test, based on 40 scratch-and-sniff cards. Each card in the set carries a different odor, which can also vary in strength or intensity. A person’s score equals the total number of correctly identified scents.
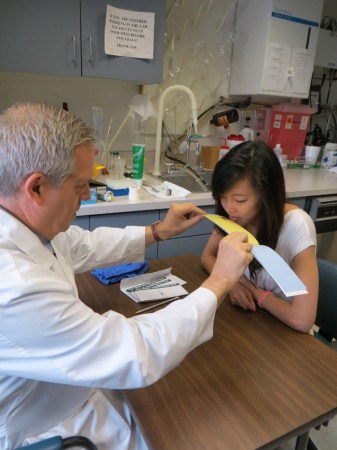
The cards allow doctors to measure how many scents people can detect and to gauge the severity of any loss of smell. Today, laboratories around the world use the University of Pennsylvania Smell Identification Test, or UPSIT.
In one project, Doty’s team used the cards to test smokers. The test revealed that the more cigarettes people smoked, the poorer their ability to detect or identify chocolate, rubber, rose, apple and other scents.
In another, Doty tested 99 people who breathed in smoke and dust during the collapse of the World Trade Center on Sept. 11, 2001. He found their sense of smell was generally not as sensitive as that of other people. The study showed certain airborne pollutants can blunt our sense of smell.
A key interest for Doty is the long-known link between a declining sense of smell and the onset of an incurable brain disorder called Parkinson’s disease. It strikes millions of mostly older people worldwide. It causes tremors, or shaking, in patients and makes it difficult for them to walk, talk, eat — and smell. So far, more than 100 studies have measured smell loss in Parkinson’s patients.
Among these individuals, “this decrease in the ability to smell things happens years before the onset of other symptoms,” Doty says. So a smell test could help diagnose the disease much sooner than is now possible. That could give patients access to early treatment and limit more severe symptoms later on.
One complication: A loss of smell occurs in patients with Alzheimer’s and other diseases that affect the brain and nerves too. So Doty is looking for differences that could help distinguish patients in the early stages of Parkinson’s disease from those with other similar conditions.
Doty’s research team is also working with patients who have begun taking medication for Parkinson’s disease. The researchers repeatedly administer smell tests to the patients and scan their brains, using an imaging device called SPECT. The scans help doctors identify whether the medication is working.
“So far, the smell tests are proving to be more sensitive than the brain scans for Parkinson’s disease,” Doty says. The initial findings suggest it may be possible for doctors to use inexpensive smell tests to diagnose Parkinson’s even before the disease shows up in far more expensive brain scans. While the research is preliminary, Doty says, it is promising.
“It’s truly exciting taking what we are learning about smell and using it to help people,” says Doty, echoing the enthusiasm Hagelin and Gouma share for scent science.
Power Words
acetone A chemical produced by the body that is detectable in people’s breath. It’s also an extremely flammable liquid solvent used, for example, in nail polish remover.
Alzheimer’s disease An incurable brain disease that can cause confusion, mood changes and problems with memory, language and problem solving.
diabetes A group of diseases that affect how the body uses glucose, a sugar that is the body’s main source of energy.
insulin A hormone produced in the pancreas (an organ that is part of the digestive system) that helps the body use glucose as fuel.
nitric oxide A chemical involved in many biological functions, including helping blood vessels relax to increase blood flow. Lung inflammation causes levels of this chemical to increase in the breath.
olfaction Sense of smell.
Parkinson’s disease A disease of the brain and nervous system that causes tremors and affects movement, memory and mood.
prototype An early working model of a device.
Word Find (click here to print puzzle)

This is one in a series on careers in science, technology, engineering and mathematics made possible by support from the Northrop Grumman Foundation.






