Extreme survival: Managing the deadly cold
Simple steps reduce risk of frostbite and hypothermia — so let the freezing fun begin

Careful planning can let you enjoy chilly activities while avoiding hypothermia, frostbite and other cold-related injuries.
Levinmatkailu/Wikimedia Commons (CC BY-SA 4.0)
Share this:
- Share via email (Opens in new window) Email
- Share on Facebook (Opens in new window) Facebook
- Share on X (Opens in new window) X
- Share on Pinterest (Opens in new window) Pinterest
- Share on Reddit (Opens in new window) Reddit
- Share to Google Classroom (Opens in new window) Google Classroom
- Print (Opens in new window) Print
By Susan Moran
Modern humans evolved in the warm tropics of Africa. Eventually, our species began to scatter into cooler climes more than two million years ago. Yet even after all that time, we still need a lot of help surviving where it is bitterly cold.
Luckily, our enlarged brains helped us create technology that can keep us as warm as a woolly mammoth, even where it’s extremely cold. But that doesn’t mean we should take our comfort for granted. Thick gloves and puffy jackets can’t protect us against every frigid environment.
Our species “is a tropical animal,” says Michael Tipton. He’s a physiologist at the University of Portsmouth in England. There, he studies how the body responds to extremely cold air and water. What he has learned helped him advise the makers of clothing and equipment for polar explorers. It also informed part of the book he co-wrote: Essentials of Sea Survival. “We have used our intellect [and] technology to move out of the tropics,” he says. Way out.
You may not be planning an expedition to the North Pole in the foreseeable future. Or to Antarctica or Mount Everest, for that matter. But explorers and winter Olympians aren’t the only ones in danger of frostbite, hypothermia and other cold-related illnesses. You can get very sick — even die — from exposure to cold temperatures, even when it’s well above freezing outside.
Whether skiing in the backcountry or jumping in a frigid mountain lake during a sweaty summertime hike, you can risk serious injury from the cold. Knowing your body’s limits is essential to having healthy outdoor adventures.
In recent years, scientists have learned a lot about how our bodies respond to extreme cold. Their knowledge is helping doctors better understand and treat symptoms of cold injuries. And that’s helping us all to stay safer.
Know the risks
There are several types of cold-related injuries and illnesses. Frostbite is the most obvious. Indeed, you can see it.
Frostbite occurs when exposure to very cold temperatures makes blood vessels shrink. This slows the flow of blood and oxygen. Air temperature, wind speed and wetness all add to the risk of frostbite.
At first the skin will redden and turn very cold. Then it will go numb, harden and turn pale. In extreme cases, ice crystals can form in affected body parts. Most often, these will be the fingers, toes, ears, nose, cheeks or chin. In the worst cases, frostbit tissues will blacken and die. This may lead to the loss of that body part.
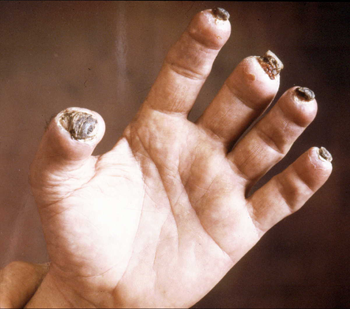
That’s what happened to the polar explorer Sir Ranulph Fiennes in 2000. He lost all the fingertips of his left hand to frostbite while trying to survive a solo walk to the North Pole. The expedition failed when his sleds fell through the ice and he had to pull them out by hand. This froze his fingers. It also brought an end to his mission. (Tipton and his colleagues tested and advised on some of the gear that Fiennes had used.)
Much less dramatic, but sometimes still severe, are non-freezing cold injuries, or NFCIs. These can develop in less than freezing temperatures. The most common NFCI is known as trench foot. Its name comes from soldiers who fought in soggy trenches during World War I. The painful condition is caused by feet remaining in cold water or mud for long periods. Affected tissues can turn blue or blacken as they die from a lack of blood supply. Feet may give off a stinky, decaying odor as tissue death sets in.
NFCIs like trench foot can be hard for doctors to spot in time. There’s no great way to test for trench foot. “You know when someone has it severely because he’ll be struggling to walk,” Tipton says. But he and other researchers are hoping to change that. They’re still trying to figure out how trench foot starts and what makes it turn severe.
At the other end of the scariness spectrum is hypothermia, which can kill. As its name implies, the body is losing heat faster than it can produce more. That makes the body’s core temperature drop dangerously low. Hypothermia typically comes from exposure to cold weather, or being dunked in very cold water.

The normal temperature for a human body is roughly 37° Celsius (98.6° Fahrenheit). Hypothermia sets in when the body falls below 35 °C (95 °F). At first, people will shiver. Then their breathing will turn slow and shallow. The victim can become sleepy or feel exhausted. As the brain fails to get enough oxygen, a person might become confused or show memory loss and become uncoordinated. The victim’s pulse also will slow and weaken. As their condition turns extreme, people can lose consciousness and appear to stop breathing.
Generally, hospitals treat hypothermia by warming the body back to a normal temperature.
But how low can the core body temperature drop before it’s too late to save someone? That’s the big question. And the answer has changed in recent years. That’s because medical experts have made new discoveries about how the human body responds to extreme cold. There also have been new advances in medical technology.
The brink of death
It turns out that the line between life and death is rather blurry.
A major milestone came in May 1999. That’s when a 28-year-old skier and medical intern named Anna Bågenholm was essentially brought back from the dead. Her body temperature had dropped to 14 °C (57 °F). That was the lowest body temperature a living person had ever been known to survive. To this day it remains a world record. (Not that she was trying to win a medal!) Until that time, doctors thought that once the core body temperature fell below roughly 15 °C (59 °F), you were a goner.

Mads Gilbert fights back tears as he describes the intensity and horror of that day nearly 18 years ago — and then the seeming miracle. He is a physician who heads the emergency medicine department at the University Hospital of North Norway in Tromsø. Gilbert led the team that rescued Bågenholm from the brink of death.
While skiing with two friends down a steep, icy gully, Bågenholm fell into freezing water. She got trapped there between rocks under a thick slab of ice. The ice had a small pocket of air. And that’s what allowed her to breathe. But her friends couldn’t pull her out, and within an hour Bågenholm stopped moving. By the time the rescue team arrived and cut her out of the water, she was no longer breathing. They could not find her pulse.
“She was clinically dead,” explains Gilbert. “No [breathing]. No circulation. Ice-cold. Dilated pupils. No signs of life.”
A helicopter carried Bågenholm to Gilbert’s hospital, where his team anxiously awaited her. Along the way, paramedics desperately performed CPR (cardiopulmonary resuscitation) on her. That’s when someone pushes down with the hands onto the victim’s chest (to push air out of the lungs) and then periodically blows air into the person’s mouth. “We didn’t know who this lady was,” Gilbert recalls. “We saw a dead body coming out of helicopter. I mean dead. Ice cold. She looked like a candle — stiff skin, waxy white.”

Gilbert and his team tried an advanced life-support procedure on Bågenholm. Doctors had only recently starting using the procedure to save the lives of patients with hypothermia. It’s called extracorporeal membrane oxygenation, or ECMO. Extracorporeal (EX-tra-KOR-por-EE-uhl) means “outside the body.” Oxygenation (OX-uh-gen-AY-shun) refers to providing oxygen, which a body’s cells need to survive. A machine sucks the blood out of the body, then filters it, warms it and pumps oxygen into it before sending it back into the vessels. With this technique, Bågenholm’s body gradually warmed.
More surprisingly, her heart started beating again.
Despite the icy ordeal, Bågenholm’s brain was fine. After many months of physical therapy, the woman was back on the mountains, hiking and skiing. She is now a radiologist, working alongside those who saved her at the hospital in Tromsø. Since her incident, several other frozen people have similarly been brought back from the brink of death as she was.
Gilbert says there’s a key lesson in that stunning “resurrection,” as he calls it. It’s a well-known saying in medicine: “You’re not dead until you’re warm and dead.” Tipton explains that especially when you’re out in the mountains, far from hospital equipment, it’s hard to diagnose death in a very cold person. That person might look dead, with a very slow heart rate, shallow breathing and no reflexes. But until you warm him or her back up you won’t know for sure.
The bottom line for us all, Gilbert advises, is to never give up.
Staying safe
You may never completely eliminate the risk of frostbite, hypothermia or some other cold-related injury — unless you stay indoors during your vacation, safely glued to your smartphone. And who wants to do that?
But you can keep your risks low by being prepared.
“There’s an old adage,” says John Castellani. “There’s no bad weather, just bad equipment. Castellani is a research physiologist at the U.S. Army’s Research Institute of Environmental Medicine in Natick, Mass. He studies how soldiers — and ultimately athletes and the rest of us — can perform well and stay safe in extreme environments.

I can vouch for the importance of good equipment. In late November 2010, I jumped into the ice-sprinkled, –0.56 °C (31 °F) Southern Ocean. I was on a reporting trip to Palmer Station, a small U.S. research site off the Western Antarctic Peninsula. I wouldn’t be alive to tell you this story if not for the gear I was wearing — a suit specially built for cold water.
I wasn’t diving in for fun. I was taking part in a safety drill. All scientists and other visitors there must do search-and-rescue training before venturing onto the ocean in inflatable boats. Despite the initial shock of hitting the frigid water, I eventually felt as comfortable as a seal. I stayed happily insulated while rolling around in the water until I was “rescued.”
“We never want to tell anybody that they can’t go out into the environment and do something,” Castellani says. “In fact, there’s no environment that people don’t go into. You just have to have the right gear.”





