Altered gene leaves people totally painfree
And that’s not a good thing
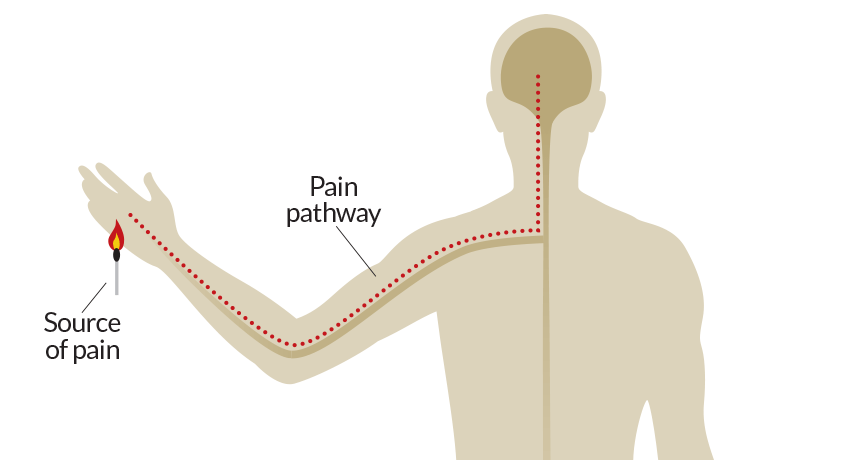
Rare changes in a certain gene can prevent a baby from developing the particular nerves designed to carry signals for pain (example depicted as red dotted line). Affected people will not feel pain, even when injured by bangs, scrapes, burns or more.
E. Otwell/ SSP
Share this:
- Share via email (Opens in new window) Email
- Share on Facebook (Opens in new window) Facebook
- Share on X (Opens in new window) X
- Share on Pinterest (Opens in new window) Pinterest
- Share on Reddit (Opens in new window) Reddit
- Share to Google Classroom (Opens in new window) Google Classroom
- Print (Opens in new window) Print
Naturally occurring changes in a previously unstudied gene can prevent people from experiencing pain. And that’s not good. It can leave them dangerously unaware of harm.
Researchers presented the finding May 25 in Nature Genetics.
The gene’s name is PRDM12. Pain is the body’s way of signaling that something is wrong. Certain mutations — naturally occurring changes — in that gene keep people from feeling pain. Robbed of this warning, affected people may fail to protect themselves from unintentional injuries. Such injuries could range from skin burns or scratched eyes to missing digits.
However, there is some good news in the finding. Better understanding of how a mutated PRDM12 gene blocks pain might one day lead to better treatments for people who suffer from too much pain.
“It’s promising, but there’s a long way to go,” says Simon Halegoua. He’s a neuroscientist at Stony Brook University in New York who did not work on the new study.
Scientists already knew that mutations in another gene caused a similar birth defect: this insensitivity to pain. In their new study, Geoff Woods of the University of Cambridge in England and his colleagues identified 11 families with mutated forms of the PRDM12 gene. The gene normally instructs cells on how to make a protein that helps pain-sensing nerve cells develop. These pain-warning nerve cells, or neurons, are called nociceptors (NO-see-SEP-terz). People born with some mutations to PRDM12 lack some nociceptor neurons that carry pain signals to the brain. The new study suggests “You need PRDM12 present to grow your pain neurons,” Woods says.
The PRDM12 protein probably helps direct the creation of nociceptor nerves as a baby develops in the womb, Woods says. But that same protein also may have a job to do even after birth. This hints that the gene plays a role in keeping fully formed pain-sensing neurons working well.
The gene’s protein seem to be present only in pain cells and their precursors, says Woods. And that’s “exciting,” he adds. He says it raises the prospect of one day developing a drug that could ultimately tamp down chronic pain without causing problems elsewhere in the body. “The more we can understand about how these nociceptors work,” he explains, “the more likely we are to have treatments for the vast numbers of people with chronic pain.”
Power Words
(for more about Power Words, click here)
chronic A condition, such as an illness (or its symptoms, including pain), that lasts for a long time.
gene A segment of DNA that contains the instructions for making a protein. Those proteins govern the behavior of a cell — or large groups of cells. Offspring inherit genes from their parents. Genes influence how an organism looks and behaves.
mutation Some change that occurs to a gene in an organism’s DNA. Some mutations occur naturally. Others can be triggered by outside factors, such as pollution, radiation, medicines or something in the diet. A gene with this change is referred to as a mutant.
neuron or nerve cell Any of the impulse-conducting cells that make up the brain, spinal column and nervous system. These specialized cells transmit information to other neurons in the form of electrical signals.
nociceptor A type of nerve cell that responds to signs of injury by telling the brain to signal the problem by triggering pain.
proteins Compounds made from one or more long chains of amino acids. Proteins are an essential part of all living organisms. They form the basis of living cells, muscle and tissues; they also do the work inside of cells. The hemoglobin in blood and the antibodies that attempt to fight infections are among the better-known, stand-alone proteins. Medicines frequently work by latching onto proteins.







