Eating disorders: The brain’s foul trickery
Science is unraveling how the brain fools some of us into eating too little — or too much

Scientists don’t yet know why certain young people become so fixated on being thin that it develops into a type of mental illness. But new research points to changes in the brain, including signals that can go awry.
tomazl/iStockphoto
Share this:
- Share via email (Opens in new window) Email
- Share on Facebook (Opens in new window) Facebook
- Share on X (Opens in new window) X
- Share on Pinterest (Opens in new window) Pinterest
- Share on Reddit (Opens in new window) Reddit
- Share to Google Classroom (Opens in new window) Google Classroom
- Print (Opens in new window) Print
Second of two parts
Georgia Woodward, of Sydney, Australia, began performing in dance groups as a child. At 12, she started acting too. To most people, her slender figure seemed natural for a dancer and actress. Even today, few realize the torments she suffered to stay so trim. She didn’t keep the weight off by exercising or dieting. Instead, she endured a mental illness. It prompted her to starve herself. And this went on year after year after year.
Her problems started when she was about 12. That’s when she began cutting calories severely. It left her hungry. All of the time. But she saw an upside to her struggles. By taking such strict control of her body she gained self-confidence. So she ate little and began deliberately purging (vomiting shortly after most meals). In time, these behaviors became familiar and even comforting.
But Woodward’s body eventually became severely — and dangerously — underweight. This worried her family. During her teen years, they left bathroom scales around the house. They also encouraged the girl to eat more. None, however, thought she needed medical help.
People “just thought that I was choosing to be skinny,” the young woman recalls. They assumed that fixing the problem would be as easy as reminding her to eat. In fact, Woodward explains, “It’s not like that at all.”

The turning point came in 2012, when Woodward was 19. She was in the bathroom, vomiting after a meal. Her partner’s mother overheard her and confronted Woodward. Only then did the teen seek help. Doctors diagnosed her as having anorexia nervosa with purging behavior. “That,” she says, “opened my eyes to the fact that I’ve had an eating disorder for a long time.”
It also meant Woodward hadn’t truly been in control of her body. Her brain had been broadcasting lies about her appearance and self-worth. Its deception had prompted her to starve herself.
Medical researchers remain puzzled over why certain young women (and some young men) develop such an unhealthy relationship with food. The good news: These same researchers are making headway in learning which signals go awry in the brains of people who suffer from eating disorders.
Coping with self-doubt
There’s much that science doesn’t know about the biology of eating disorders. But slowly, researchers have begun filling in the puzzle, one piece at a time.
Some genes have been linked to a heightened risk of developing an eating disorder. But the illness may not emerge unless some mix of stresses and other factors also occurs.
A number of factors can put somebody over the edge. Many of these will be familiar to most preteens and teens. It may be a pressure to diet. It could be anything that prompts initial weight loss, such as an illness or death in the family, says Angela Guarda. She directs the eating disorders program at the Johns Hopkins School of Medicine in Baltimore, Md. Another possible trigger: being unhappy with one’s appearance, often starting around puberty.
Certain chemicals ferry signals around the brain. These messengers are called neurotransmitters. Some play important roles in stress, mood and appetite. Experts believe that eating disorders may develop when levels of certain neurotransmitters become unbalanced. One of them — serotonin — has a central role in other mental disorders, such as anxiety and depression.
Brain scans now reveal that some cells do not swap serotonin signals properly in people with anorexia nervosa and bulimia nervosa. As a result, their brains get too little of this chemical.

Anorexia nervosa causes its sufferers to deliberately starve themselves, often while exercising too much. Bulimia nervosa causes its victims to gorge on food — and then to deliberately vomit it up a short while later. Research has linked both disorders to anxiety.
Indeed, these eating behaviors seem to help their victims cope with anxiety —but only at first. Any comfort these behaviors bring will be short-lived. And then the cycle of feeling badly about oneself and trying to ‘fix it’ through improper eating habits will repeat itself.
As James Lock explains it: “There are people who overeat when they’re anxious and people who under-eat, and people in the middle.” Lock directs an eating-disorders program at Stanford University in Palo Alto, Calif. He also has coauthored several books on these problems. (One of them for parents is “Help Your Teenager Beat an Eating Disorder.” Guilford Press is issuing a second edition of it in 2015.)
Low serotonin is not, however, the only culprit.
Problems in dealing with “rewards”
Among people with eating disorders, something goes askew in a region of the brain known as the reward center. This part of the brain processes the good feelings that can come when we get smiles, gifts or compliments. When we receive such a reward, our brain releases dopamine. No wonder it’s often called the ‘feel-good’ chemical. But pathways carrying that signal seem to be miswired in people with eating disorders, studies show.
When it comes to dopamine and serotonin — and even other chemical messengers in the brain, Lock says: “They’re all interacting.” So you can’t fully separate out the effects of each. It’s not like they are “on separate railroad tracks,” moving about the brain individually, he explains.Research shows that people with anorexia also tend to be extra sensitive to rewards. “They get overwhelmed by what the rest of us would find to be an OK stimulus,” says Lock. Even just the basic process of eating can be overwhelming and can trigger anxiety, he says.
What’s worse, studies suggest that people with anorexia become more sensitive to the rewards they receive when they restrict how much they eat, says Guido Frank. He’s a brain researcher in Denver who specializes in eating disorders. Frank is based at the Children’s Hospital Colorado.
Chronically starving the body actually changes the way the brain processes rewards in people with anorexia. He says that makes it even harder for them to eat normally again.
In contrast, people with bulimia seem to be under-stimulated by rewards.
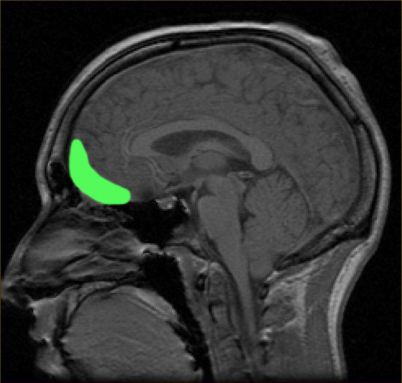
Brain differences
The size and shape of certain brain regions are different in people with eating disorders. Frank led two 2013 studies that illustrate this. Both showed important structural differences in certain brain regions.
Take the orbitofrontal cortex. This brain region sits just between the eyes. It is larger than normal in young people and adults with anorexia nervosa and bulimia nervosa. Study participants who had recovered from anorexia showed this same enlargement.
This may be an important clue: The affected region includes a structure called the gyrus rectus (JY-rus REK-tus). It plays an important role in regulating how much we eat.
Frank and his fellow researchers found that a second structure, the right insula, also was enlarged in patients with anorexia and in people who had recovered from the illness. In patients with bulimia, the left insula was larger than in healthy people.
The left and right insula are tucked deep inside the brain. The insula tell us what taste we just experienced. It then connects with other brain regions to allow us to feel pleasure or dislike about that taste. Now we can make a decision whether we want more of a particular food, says Frank. The insula also integrates how we feel about our body and our sensation of pain.
Whether these altered regions help trigger eating disorders or instead are caused by them remains unknown, Frank says.
But the new studies do show that these illnesses have a strong basis in brain biology, he says. And those biological origins of eating disorders may occur early in brain development.
These data can help “people to understand what these kids and their families are up against,” Frank says. “It’s not ‘just the fear of weight gain’ and ‘just the fear of getting fat,’” he says. “It’s also something clearly biological that makes it really hard for them to go back to normal.”
Beyond the brain
In this video, a dentist describes the potential effects of eating disorders on teeth. Cavan Brunsden |
Eating disorders affect much more than just the brain, of course. People with anorexia lose so much muscle that even the heart (which is made of muscle) can shrink and weaken. Then the heart may no longer pump blood properly.
One result is that blood may not circulate through the body efficiently. This explains why a person with an extreme case of anorexia nervosa may always feel cold. (This was true for Rae Smith — introduced in part one of this series — at the height of her illness.) Poor circulation also causes heart rate and blood pressure to fall. Ultimately, it creates a high risk for heart failure. Indeed, some 80 percent of patients with anorexia report heart problems.
Another dangerous impact: Anorexia can lead to thinning and loss of bone. This condition is called osteoporosis (OSS-tee-oh-puh-ROE-sis). The term is Greek for porous bones. Typically, osteoporosis occurs when people are in their 60s or older. However, young people who severely restrict their calories, even just for six months, can begin to experience bone thinning.
In severe cases, a 30-year-old’s bones will look like those of someone over 80, says Linda Smolak. She is an expert on eating disorders at Kenyon College in Gambier, Ohio. Indeed, those young bones can break, Smolak points notes. A July 2014 study in the International Journal of Eating Disorders found that young people with anorexia face a greatly elevated risk of bone fracture. This was true even among anorexics whose bone density otherwise seemed normal.

Many other problems are associated with bulimia. Because people with this disease binge and purge repeatedly, they often become severely dehydrated.
Their body also lacks minerals that it needs, including sodium, potassium and chloride. Those mineral changes can throw off the balance of electrolytes in the body. (Electrolytes are minerals in the blood and other bodily fluids that carry electrical charges.) When electrolytes are out of balance, major organs — including the heart and kidneys — may not work properly.
The stomach acids brought up when people repeatedly purge can wear away or pit the enamel on teeth. Far worse, these acids can cause the stomach and esophagus to bleed. Death can follow.
Lifeline
Treating eating disorders usually requires some form of mental-health counseling. This type of treatment is called cognitive behavior therapy. It helps people explore the roots of their negative thoughts or behaviors. In time, therapy can teach a patient how to think, behave and cope in more positive ways.
Anxiety, depression and drug abuse often accompany eating disorders. This means that any treatment also may require dealing with these extra issues. Luckily, eating disorders often can be treated. This help includes the kind doctors, therapists and dieticians (experts on nutrition) provide. Together, such experts can help someone work through medical issues and develop healthy eating habits.
Still, recovery will likely be both long and difficult. Sarah Robertson says her recovery from anorexia remains an ongoing process. After being diagnosed in 2011 at age 25, the British woman began treatment at a facility near her home in Staffordshire. By mid-2012, she had become medically stable. Today, she is still working to reach a healthy weight.
“I know I haven’t beaten it,” says Robertson of her illness. “It took 20 years to develop; it’s not going to go within two.” But Robertson is enjoying food again, and she now finds it easier to go out to eat with friends.
Online help
Woodward, now 21, has found a lifeline through a free app for smartphones. It’s called Recovery Record (www.recoveryrecord.com). More than 4,000 eating-disorder experts use the app to help their patients. Another 100,000 people with eating disorders and exercise addiction are using the app on their own. It helps people in recovery develop coping skills. With this app, they can plan their meals, log what they eat and more.

The app helps Woodward at every stage of her treatment. She logs her meals regularly to make sure that she eats enough to stay healthy. This is important because people with anorexia often skip meals or eat just enough to get by (perhaps a slice of bread). She also records her progress and setbacks.
The information that Woodward plugs in allows her psychologist to monitor her progress between meetings. When difficult situations arise, it also alerts her doctor. Woodward says the app has been“phenomenal” at keeping her on track.
Recovery Record also has helped Erin Shanks, 25, who lives in St. Louis, Mo. Shanks discovered the app while secretly battling anorexia. She credits the cell-phone program with encouraging her to finally seek professional help. “It was my first social support,” she says. “I was trying to get help and didn’t know how.”
Early in her recovery, Shanks says she would forget to eat. The reminders provided by the app were a big help. Despite the small setbacks she still experiences, Shanks believes she is on the road to a full recovery from anorexia.
“I always pull myself back up and I tell myself I can handle it.” When she emails her dietician or therapist, Shanks says, “My ending line is always, ‘I can do this.’”
Power Words
addiction The uncontrolled use of a habit-forming drug or uncontrolled and unhealthy habit (such as video game playing or phone texting). It results from an illness triggered by brain changes that occur after using some drugs or engaging in some extremely pleasurable activities.
anorexia nervosa An eating disorder that involves self-starvation and excessive exercise to lose weight.
anxiety A nervous disorder causing excessive uneasiness and apprehension. People with anxiety may even develop panic attacks.
app Short for application, or a computer program designed for a specific task.
behavior The way a person or other organism acts towards others, or conducts itself.
binge-eating disorder An eating disorder in which a person eats massive amounts of food, often in secrecy.
body image The impression individuals have about how attractive or comfortable they feel about the way their body is shaped — or how it looks when they view it in a mirror.
brain scan The use of an imaging technology, typically using X rays or a magnetic resonance imaging (or MRI) machine, to view structures inside the brain. With MRI technology — especially the type known as functional MRI (or fMRI) — the activity of different brain regions can be viewed during an event, such as viewing pictures, computing sums or listening to music.
bulimia nervosa An eating disorder involving overeating followed by purging (deliberately vomiting up a meal).
circulation (in biology) A term that refers to the pumping of blood through the arteries, and smaller types of vessels (and from there into other organs and tissues).
cognitive A term that relates to mental activities, such as thinking, learning, remembering and solving puzzles.
dehydrate To lose a large amount of water.
density A measure of the consistency of an object, found by dividing the mass by the volume.
depression A mental illness characterized by persistent sadness and apathy. Although these feelings can be triggered by events, such as the death of a loved one or the move to a new city, that isn’t typically considered an “illness” — unless the symptoms are prolonged and harm an individual’s ability to perform normal daily tasks (such as working, sleeping or interacting with others). People suffering from depression often feel they lack the energy needed to get anything done. They may have difficulty concentrating on things or showing an interest in normal events. Many times, these feelings seem to be triggered by nothing; they can appear out of nowhere.
dietician An expert who works out what an individual should eat to attain and maintain a healthy weight. Dieticians also can work out meal plans to help people with special medical problems, such as heart disease and diabetes.
dopamine A neurotransmitter, this chemical helps transmit signals in the brain.
eating disorder An illness of the mind involving dangerously unhealthy patterns of eating and weight loss or gain.
electrolytes Minerals in the blood and other bodily fluids that carry electrical charges.
enamel The glossy, hard substance that covers a tooth.
esophagus The tube that starts at the back of the throat and carries food, liquids and saliva to the stomach.
factor Something that plays a role in a particular condition or event; a contributor.
fracture (noun) A break. (verb) To break something and induce cracks or a splitting apart of something.
gene (adj. genetic)A segment of DNA that codes, or holds instructions, for producing a protein. Offspring inherit genes from their parents. Genes influence how an organism looks and behaves.
heart failure A weakening of the heart that leads to its inability to pump enough blood to meet the needs of its tissues. It does not mean the heart has stopped. But if left untreated, heart failure can lead to death.
insula A structure buried deep inside the brain that is thought to play a central role in responding to one’s surroundings and generating emotional responses. There is one on each side of the brain.
media (in sociology) A term for the ways information is delivered and shared within a society. It encompasses not only the traditional media — newspapers, magazines, radio and television — but also Internet- and smartphone-based outlets, such as blogs, Twitter, Facebook and more. The newer, digital media are sometimes referred to as social media.
mineral The crystal-forming substances, such as quartz, apatite, or various carbonates, that make up rock. (in physiology) The same chemicals that are needed by the body to make and feed tissues to maintain health.
neurotransmitter A chemical substance that is released at the end of a nerve fiber. It transfers an electrical signal to another nerve, to a muscle cell or to some other structure.
osteoporosis A disease in which bones become weak, brittle and at risk of breaking.
psychology The study of the human mind, especially in relation to actions and behavior. Scientists and mental-health professionals who work in this field are known as psychologists.
puberty A developmental period in humans and other primates when the body undergoes hormonal changes that will result in the maturation of reproductive organs.
purge To intentionally remove something. (in eating disorders) To intentionally vomit after eating to keep the calories in food from being used by the body. It is a harmful behavior practiced by some people with eating disorders, especially those suffering from bulimia nervosa.
reward center A region of the brain that processes the pleasant reactions we get when we get smiles, gifts, pleasurable stimuli (including food) or compliments.
serotonin A chemical present in blood that constricts blood vessels and communicates signals in the brain and nervous system.
smartphone A cell (or mobile) phone that can perform a host of functions, including search for information on the Internet.
social media Internet-based media, such as Facebook, Twitter and Tumblr, that allow people to connect with each other (often anonymously) and share information.
social network Communities of people that are interrelated owing to the way they relate to each other, such as sharing details of their life and interests on Twitter or Facebook, or perhaps belonging to the same sports team, religious group or school.
stimulus (plural: stimuli) Something that prompts a response in a living organism or in a controlled environment (including a chemical or physical test system).
stress (in biology) A factor, such as unusual temperatures, moisture or pollution, that affects the health of a species or ecosystem.







