Brain’s immune system can play role in weight gain
At least in mice, certain immune cells in the brain can make a fatty diet more fattening

When mice eat high-fat diets, they can become obese. That might be partly due to immune cells in their brains, a new study shows.
Georgejason/istockphoto
Share this:
- Share via email (Opens in new window) Email
- Share on Facebook (Opens in new window) Facebook
- Share on X (Opens in new window) X
- Share on Pinterest (Opens in new window) Pinterest
- Share on Reddit (Opens in new window) Reddit
- Share to Google Classroom (Opens in new window) Google Classroom
- Print (Opens in new window) Print
Maintaining body weight isn’t as simple as burning off all the calories eaten in a day. The brain plays an important role. It determines what you eat, how much and when. And the brain’s immune cells contribute, too, a new study in mice shows. Turning on these cells can make a fatty diet more fattening. Getting rid of those cells, known as microglia, can make the animals eat less and gain less weight.
These microglia can inflame a particular area of the brain. And in mice, this process could make the animals gain weight — even when they weren’t eating a fatty diet.
“I think it’s really neat,” says Kate Ellacott, who was not involved in the study. “This is the first time anyone’s shown if you change the way microglia can behave — if you make them more inflammatory — you can impact bodyweight.” Ellacott is a neuroscientist, someone who studies the brain, at the University of Exeter in England.
The immune system is a collection of cells that can move throughout the body to help fight infection and damage. When a part of the body is stressed or injured, the hurt part sends out chemical distress calls. Those messages are like an alarm. They tell immune cells where to swoop in so that they can destroy damaged cells or gobble up germs.
Along the way, immune cells cause inflammation. This response can include redness and swelling. People often think of inflammation as a swollen knee or the redness surrounding a cut. Here, Ellacott points out, the immune system works to “restore balance.” The immune system tries “to repair tissues and get back to normal,” she explains.
But sometimes, inflammation sticks around for the long term, even when it’s not supposed to. Such chronic inflammation does not have to include redness. But it will cause harm. “If you have a disease where inflammation never goes away, you can get damage to the tissue,” she points out.
One condition where chronic inflammation occurs is obesity. Eating a high-fat diet for a while makes animals gain weight and activates their immune cells, says Joshua Thaler. He’s an endocrinologist (someone who studies the hormones in the body) and a neuroscientist. He works at the University of Washington in Seattle. There, his team performed the new study.
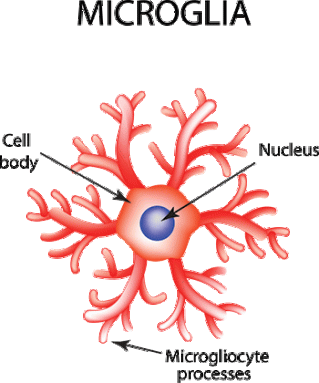
The brain is full of cells called neurons. But they aren’t alone. A variety of other cell types live there too, Thaler notes. For a while, scientists thought some of these cells, called glia (GLEE-ah), were just there to support neurons and to hold them together. (In fact, “glia” comes from the Greek word for glue.) But glia are far more than just brain glue. Some of them, called microglia, act as an immune army in the brain. They move into injured areas and can turn on inflammation when things go wrong.
Thaler’s team already had found that one brain area gets inflamed when mice eat a high-fat diet. Called the hypothalamus, this brain area helps to regulate how much mice — and people — eat. They even showed similar changes in the brains of people with obesity.
Could the microglia in the hypothalamus be the reason why? To find out, Thaler and his colleagues fed high-fat diets to more mice. Then they gave some of these mice a drug that killed off microglia. Without these immune cells, those mice gained less weight and ate less food. But losing their microglia had no effect on mice dining on low-fat chow.
The researchers wanted to make sure microglia were causing the inflammation that led to weight gain. So they deleted a gene — a set of cellular instructions. Microglia use this gene to make their inflammatory signals. The treated mice gained less weight on a high-fat diet, just as in the mice with no microglia at all.
If stopping inflammatory signals made mice gain less weight, more inflammation might have the opposite effect. Thaler’s group decided to test that idea. They worked with mice that were unable to make an important inflammation-fighting molecule. These mice developed inflammation in their brains. They also gained weight — even when they weren’t on a high-fat diet! That confirmed that brain inflammation alone could contribute to obesity.
Thaler and his colleagues published their findings July 5 in the journal Cell Metabolism.
Calling in the immune cavalry
Microglia are full-time brain residents. “They’re always there,” Ellacott says. These cells move to wherever the brain needs them.
When mice eat a high-fat diet, the hypothalamus recruits microglia. And these immune cells then call for backup. In the new study, some of those backup immune cells had come from a mouse’s bone marrow.
Usually, immune cells in the marrow can’t reach the brain. There’s a barrier between the blood and the brain that stops them. That blood-brain barrier exists to keep potentially dangerous cells and other foreign substances from getting in.
Somehow, a high-fat diet let those marrow-based backup cells break into the brain.
Some scientists had seen immune cells getting into other organs after a high-fat diet, Thaler notes. But his group has now shown it also happens in the brain. “I was not a believer that the [immune cells] were going to come marching into the brain,” he recalls, so “it was a bit of a surprise.”
Scientists might someday be able to reduce inflammation by targeting the microglia, Ellacott says. If they can develop a drug that works this way in people, scientists might use it to treat all types of brain diseases linked with inflammation, not just obesity.
Microglia in the brain may contribute to weight gain, Thaler says. “But clearly they aren’t the whole story.” Turning off the microglia, or stopping them from sending inflammatory distress calls, causes mice to gain less weight. But in the end, those mice still became overweight. And while mice with brain inflammation gained weight on even a low-fat diet, he notes that they never got as fat as did the mice downing high-fat chow.
The brain’s immune system may be a part of the obesity story, Thaler says, “but there’s clearly more we need to learn.”





