Good germs lurk in gross places
The secret superpowers of poop, dog drool and snot

Dogs bring dirt into our homes. And that can be a good thing, scientists find. Kids that grow up in homes with dogs can be healthier. Pets are just one unexpected source of health-promoting germs.
Willbrasil21/iStockPhoto
Share this:
- Share via email (Opens in new window) Email
- Share on Facebook (Opens in new window) Facebook
- Share on X (Opens in new window) X
- Share on Pinterest (Opens in new window) Pinterest
- Share on Reddit (Opens in new window) Reddit
- Share to Google Classroom (Opens in new window) Google Classroom
- Print (Opens in new window) Print
Everybody poops. But we don’t usually like to talk about it. “Normally we flush it down the toilet and get away from it as fast as we possibly can,” observes Ari Grinspan. But, he adds, “there is a richness and goodness associated with poop.”
Grinspan knows what he’s talking about. He is a doctor at Mount Sinai Medical Center in New York City. And he regularly uses poop as medicine. The procedure, called a fecal transplant, isn’t for everyone. But “in the right patient, in the right setting,” he says, poop can improve a person’s health.
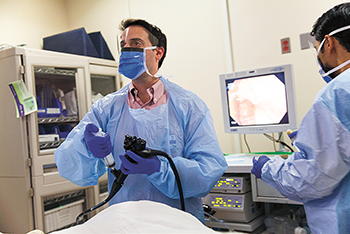
That’s because human feces contain trillions of bacteria. These tiny germs live inside all of us, forming communities called microbiomes (My-kro-BY-ohms). Each microbiome is a miniature ecosystem full of different species. These communities exist on our skin, in our noses and elsewhere, especially in our guts. In a healthy person, these bugs cause no harm. They even can help keep the body healthy.
Sometimes, though, dangerous microbes invade or take over. When bad guys overrun the community, they may cause an infection. Or they might make chemicals that harm other systems in the body. In both cases, the human host will suffer.
In many human diseases, the gut microbiome is out of whack. Getting it back to normal might treat or even cure the disease. And one way to do that is to put into the sick person’s intestines a sample of good germs from the feces of a healthy person.
Poop isn’t the only disgusting substance with the potential to promote health. A team of researchers in Canada has found that dogs are good for babies’ health — not because they’re cute and lovable, but because they’re dirty. When babies grow up around dog drool, fur and muddy paw prints, they develop healthier gut microbiomes. And a German research team probing people’s noses found a surprise in the microbiome there. It was a brand-new antibiotic. ‘Snot bad!
From yellow soup to poop milkshakes
The healing power of poop is not a new idea. In 4th-century China, a doctor named Ge Hong described treating diarrhea with an unusual concoction. It was a drink made from the feces of a healthy person. This so-called “yellow soup” remained a part of Chinese medicine for centuries.
However, Western medicine has only fully accepted the technique as treatment for one condition. That’s a potentially deadly infection called Clostridium difficile. It causes diarrhea and extreme pain in the gut. Years of research have shown that a fecal transplant is a safe and effective cure for this disease. In the United States, doctors aren’t allowed to use fecal transplants to treat anything else. The only exception is if they are testing treatments as part of a human trial.
But in Australia, the rules are different. Thomas Borody is a doctor there who founded the Centre for Digestive Diseases in Sydney. He has been giving people fecal transplants for various conditions, including C. difficile infection, since the late 1980s. Early on, he was one of a handful of doctors experimenting with the procedure. “I’ve been laughed at for a long time,” he says. But he continued to perform fecal transplants anyway. He’s done thousands of them. “A lot of things are gross in medicine,” he says. People who are sick don’t care if a treatment is icky. They just want to get better.
Borody has treated illnesses called Crohn’s disease and colitis. In these conditions, the intestines swell with inflammation and may bleed. People may have diarrhea, constipation or painful cramps. Many doctors consider both conditions to be incurable. But many of Borody’s patients feel cured and stay off treatment for years. Other doctors who once scoffed at him are starting to change their minds, he says.
Still, stories from individual patients aren’t solid proof that the technique works. Researchers are still studying whether fecal transplants can help people with these conditions.
Borody believes fecal transplants could treat a host of conditions. Autism is one of them. People with autism often have trouble speaking and interacting socially. Many also have constipation and other gut problems. Sidney Finegold is a doctor at the VA Greater Los Angeles Healthcare System in California. He found two types of gut bacteria that might be tied to certain cases of autism. He did a study showing that an antibiotic, which kills bacteria, could temporarily lessen autism symptoms.
But antibiotics destroy good bacteria as well as bad. In contrast, Borody thinks, a fecal transplant might kill bad bacteria while bringing in good ones. To test this, he and his colleagues recruited 18 children with autism. They treated each of them with purified fecal bacteria.
“We gave it to them in a chocolate drink,” says Borody. But don’t barf just yet. The team carefully screened donors and their stools for disease. Next, they mixed the poop with purified salt water. Then they filtered out everything potentially harmful (or smelly). The result was an odorless, tasteless liquid packed with healthy bacteria. Then they mixed in a chocolate flavoring.

Kids drank this concoction daily for eight weeks. During and after the treatment, parents filled out questionnaires on their kids’ symptoms. Gut conditions (such as constipation) improved, they reported. Some symptoms of autism seemed to improve as well.
The researchers published the results in January in the journal Microbiome. However, “it was a very, very small study,” notes Grinspan. He was not involved in the trial. Also, he points out, all children with autism received the same treatment. In a future study, the researchers should give some kids a fake treatment, called a placebo (Pla-SEE-bo), he says. This could help show whether any improvements are really due to the poop therapy, not just to the kids’ or parents’ expectations.
Birthing fluid and dog drool
Doctors such as Grinspan and Borody use fecal transplants to repair a microbiome gone bad. It would be even better, however, if people never fell sick in the first place. So what’s the secret to keeping your gut microbiome healthy? There are likely many factors. But researchers know that a baby’s first experiences can matter a lot.
Birth is a messy affair. There are blood, fluids and plenty of germs. During a baby’s trip through the birth canal, microbes from its mom’s body hop on board. They move into the baby’s gut. Even before birth, microbes from mom may sneak into her baby. In general, the more bacteria, the merrier.
“A baby needs to be exposed to microbes,” says Anita Kozyrskyj. She works at the University of Alberta in Edmonton, Canada. As a pediatric epidemiologist (Ep-ih-dee-me-OL-oh-gist), she studies patterns of disease among children. Exposure to microbes trains a baby’s immune system to fight bad germs and leave good ones alone. It also helps build up a diverse, healthy community of microbes in the baby’s body.
Missing out on microbes may affect a baby’s’ future health. For example, babies born in a procedure called a C-section never travel through a mom’s birth canal. Instead, a doctor cuts into the mother’s belly to remove the baby. Later in life, these babies may be more likely to have asthma, food allergies and obesity.
One team of researchers in New York City tried something unusual. (Okay, it’s also a little gross.) After a C-section, they swabbed each of four babies with fluid from its mom’s birth canal. This helped make the babies’ microbiomes more similar to those of babies born naturally, they found. This was a very small, early study. Still, notes Kozyrskyj, who was not involved, the results seem promising.

Her team is now looking at another common source of microbes: dogs and other furry pets. In a large group of 746 families with new babies, they looked at which families owned furry pets before and after the baby’s birth. They compared the gut microbiomes of babies from these families to those from families without furry pets.
Gut microbes, you’ll recall, come out in poop. To find out what kinds of microbes had moved into these babies’ guts, Kozyrskyj’s team had a messy job to do. They collected poopy diapers at each home.
It turns out that living with a dog before or after birth is good for a baby’s microbiome. All that dog hair, drool and dirt help a baby develop a diverse community of germs. And a diverse microbiome is a healthier one. “Babies had many more species [of microbes] when dogs were around than when they were not,” says Kozyrskyj. Even if the family owned a furry pet during pregnancy but not after birth, the baby still showed benefits.
Previous studies had shown that babies who grow up around dogs and farm animals are less likely to develop allergies. The microbe diversity Kozyrskyj’s team found may help explain this fact. Cats do not seem to provide the same protection. But if you own a cat, don’t despair. Kozyrskyj suspects that dogs are better for the microbiome because they spend more time outside. So they track in germs from outdoors. A cat that goes outside a lot may offer similar benefits.
Nosing around
As Kozyrskyj’s team collected poopy diapers, another team of researchers was peering into people’s noses. No, they weren’t looking for juicy boogers. They wanted to learn about the nose microbiome, says Bernhard Krismer. He works at the University of Tübingen in Germany. As a microbiologist, he studies microbes and their communities.
It turns out the nose is not an easy place to live, notes Krismer. Food for microbes is hard to come by. So bacteria that live there have to work hard to survive. One way is to kill off their neighbors. Krismer’s team discovered that one nose-dwelling bacterium does just that. Its name is a mouthful: Staphylococcus lugdunensis (STAF-uh-lo-KOK-us LUG-dun-EN-sis). This microbe makes a powerful bacteria-killing substance known as lugdunin. Last year, Krismer’s team described discovering this new antibiotic.
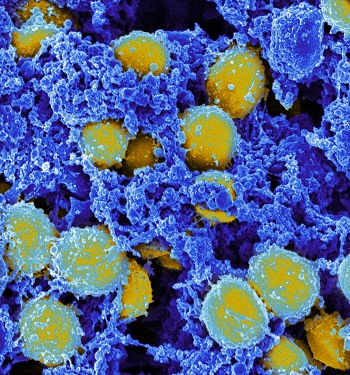
“We were very surprised,” he recalls. His team had not expected to find an antibiotic. But they realized how important the discovery could be to medicine. People regularly use antibiotics to prevent or treat infections. You may take them for an ear infection. Or you may smear some on a cut or scrape. But many common antibiotics don’t work as well as they once did. That’s because some types of bacteria have become resistant. They have found ways to protect themselves against these drugs. (One factor driving this problem is that people use antibiotics too much, Krismer says. For example, you should only put antibiotic cream on a scrape if it’s already infected.)
Researchers have to keep developing new antibiotics to fight the resistant types (or strains). Lugdunin successfully kills the bacterium Staphylococcus aureus, which also lives in the human nose. A resistant strain of this bacterium, called MRSA, can cause a life-threatening infection.
You may already have lugdunin in your nose. S. lugdunensis shows up naturally in one out of every 10 people. But even if you’re a carrier, you can’t use your boogers as a natural remedy. “Bad idea,” says Krismer. “The amount you can get by picking your nose is so low it wouldn’t help anything.” Plus, S. lugdunensis itself can cause an infection if it grows out of control.
Krismer and his team hope to partner with a company to produce lugdunin for medical use. Most likely, they would make an antibiotic cream containing this substance.
Giving good germs more respect
The lugdunin discovery shows that our own bodies may be a rich source of new potential drugs. Other microbes living in the human body also likely produce powerful antibiotics. This type of activity could explain why fecal transplants work. A healthy human gut already contains substances that fight off bad bacteria. Even though doctors don’t yet know exactly what these substances are, they can use a fecal transplant to help sick patients.

Some people fear germs of all kinds. They scrub their hands and household surfaces regularly with germ-killing products. They teach their kids to avoid dirt or sanitize their hands after petting a dog or cat. But researchers are realizing that there’s such a thing as being too clean. The body needs a diverse community of microbes to stay healthy. “If a dog licks you, I would not use a sanitizer,” says Kozyrskyj. “You can wash it off with water.”
Grinspan agrees that it’s a good idea to avoid using antibacterial soaps. These products destroy good bacteria along with the bad. He also says, “I tell my kids that playing in the dirt is okay.”
Next time you flush the toilet, pet a dog or blow your nose, think of the good germs growing in and on your body. Then wash your hands — but stick to regular soap.






