Kids now getting ‘adult’ disease
More kids are developing diabetes, and obesity is a major reason why.
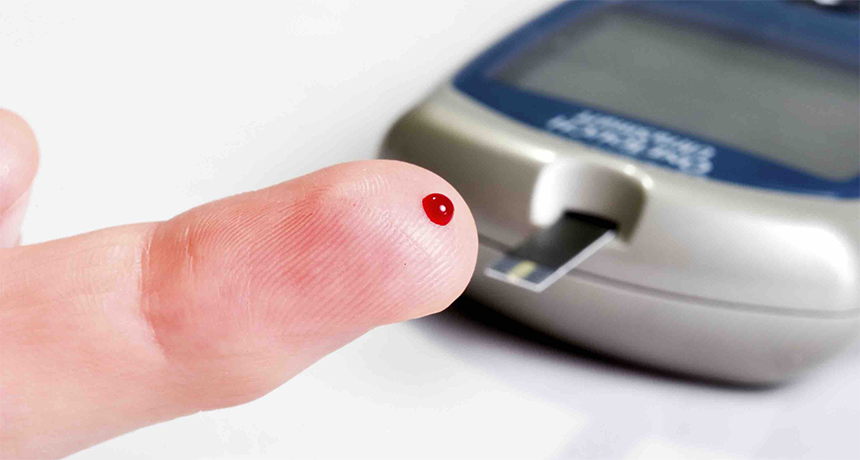
After they’re diagnosed and for the rest of their lives, type 1 diabetics need to regularly test their blood sugar levels with a pinching tool that draws a little blood. They also have to give themselves shots of insulin several times a day.
EvgenyB/iStockphoto
Share this:
- Share via email (Opens in new window) Email
- Share on Facebook (Opens in new window) Facebook
- Share on X (Opens in new window) X
- Share on Pinterest (Opens in new window) Pinterest
- Share on Reddit (Opens in new window) Reddit
- Share to Google Classroom (Opens in new window) Google Classroom
- Print (Opens in new window) Print
By Emily Sohn
When she was 9 years old, Ann Albright went to the doctor with odd flulike symptoms. She was exhausted. She had to go to the bathroom frequently in the middle of the night. She was always thirsty. Even her vision was blurry.
After a few tests, the doctor pulled Albright’s mother aside.
“I still remember it very vividly,” says Ann Albright, now more than 40 years later. “My mom left the room with the doctor and came back in with tears running down her cheeks.”
The verdict: diabetes, a disease that affects the way people process food.
At the time, the 1960s, the diagnosis meant that young Ann would never have the carefree childhood her mother wanted for her. For the rest of her life, she would have to give herself shots several times a day. She would need to be very careful about what she ate. And she might not realize all of her dreams in life.
“In the era I was diagnosed, most people were told they’d have a shorter life span,” Albright says. “As a little girl with diabetes moving into adulthood, I wondered would I be able to have kids? Would I be able to have a life?”
Science has come a long way since then, says Albright, partly as a result of her own efforts: She’s now a doctor and diabetes researcher at the Centers for Disease Control and Prevention in Atlanta. Since her diagnosis, researchers have developed better technologies, more effective medicines and a sharper understanding of how diabetes works.
Despite the advances, though, scientists still can’t answer a lot of basic questions about what causes diabetes. There still is no cure. And living with the disease remains difficult.
“Everything changes” after a diabetes diagnosis, says Ali Reed, a pediatric endocrine fellow at the University of California, San Francisco. “Life becomes more complicated.”
What’s more, diabetes is on the rise — in both adults and kids. One version of the disease, called type 2 diabetes, is increasing at an especially alarming rate.
Scientists have linked type 2 diabetes with obesity. So now, more than ever, doctors are urging young people to start developing healthy habits as early as possible.
Breakdown
Diabetes refers to a group of diseases, but there are two main kinds: type 1 and type 2. In both types, the trouble begins with the body’s ability to deal with sugar.
Sugar is the body’s main fuel source. When you eat, your digestive system breaks down your food into basic parts, including proteins, fats and a simple sugar called glucose. Glucose gets absorbed through the intestines. From there, it enters the bloodstream. Circulating blood delivers glucose to all the cells, which convert it into energy.
At least, that’s what’s supposed to happen. In people with diabetes, however, sugar can’t get from the bloodstream into the cells. A hormone, or messenger molecule, called insulin is normally responsible for that transfer. But in diabetics, insulin doesn’t do its job.
As a result, sugar builds up in the bloodstream. When levels of sugar in the blood stay high, the condition is called chronic. And for reasons scientists don’t yet understand, chronically high blood sugar can lead to blindness, kidney damage, limb amputations, heart attacks and more.
“It’s not a death sentence, but it’s a very serious disease,” Albright says.
Two types
Exactly how diabetes affects a patient’s life depends in part on which type of diabetes a person has. There are important differences between the two main types.
Type 1 diabetes is the kind Albright has. In this version of the disease, the body stops producing insulin. Symptoms usually begin in kids or teenagers.
After they’re diagnosed and for the rest of their lives, type 1 diabetics need to regularly test their blood sugar levels with a pinching tool that draws a little blood. They also have to give themselves shots of insulin several times a day to control blood sugar levels. So far, scientists don’t know how to prevent type 1 diabetes.
Type 2 diabetics make insulin, but their bodies don’t use the hormone properly. Type 2 diabetes is far more common than type 1, and most people who have type 2 are adults. These days, though, more and more kids are coming to their doctors with symptoms of type 2 diabetes.
 |
|
Doctors already know that adults who develop type 2 diabetes tend to be overweight or obese. And as kids have become increasingly overweight, the disease has started appearing at younger and younger ages.
|
| Shorrocks/iStockphoto |
As recently as a decade ago, type 2 diabetes was called “adult-onset” because kids just didn’t get it.
“When this disease we used to only see in adults started happening in adolescents, it was just shocking to people,” Albright says. “Pediatricians just didn’t know what to do.”
Healthy living
Doctors already knew that adults who develop type 2 diabetes tend to be overweight or obese. (Scientists can’t yet explain why.) And as kids have become increasingly overweight, the disease has started appearing at younger and younger ages.
In the United States, two out of three adults are now overweight, according to the CDC. Nineteen percent of kids between the ages of 6 and 11 are overweight, compared with 7 percent just 20 years ago. Over the same period, the proportion of overweight teens rose from 5 percent to 17 percent.
(You can find out whether you are overweight by plugging numbers into a calculator at an online site. Also, see the sidebar “Understanding Body Mass Index” at the bottom of this article.)
Like their type 1 peers, type 2 diabetics have to monitor blood sugar levels. But they often rely on drugs instead of insulin shots. Frequently, they can get the disease under control by simply exercising more and eating reasonable portions of healthy foods.
“We now know that we can prevent or postpone type 2 diabetes by having [adults] at very high risk lose 5 to 7 percent of their body weight,” Albright says.
Scientists don’t yet know whether the same is true for overweight kids. The trend is so new that CDC researchers are still working to gather basic information about how the disease works in young people.
But it can’t hurt to play soccer instead of video games, and to choose fruits and vegetables over junk food.
“There’s no harm in having healthier lifestyle habits,” Albright says. “Get to know what’s going into your body. Make it fun.”
Seeking answers
Weighing more than you should doesn’t mean you’re doomed to develop diabetes. The disease is far more complex than that. And while research has come a long way, plenty of questions remain.
Doctors don’t know, for example, why certain ethnic groups have particularly high rates of diabetes, including American Indians, Hispanics and African Americans. Nor can doctors say for sure why the chances of getting diabetes go up if your parents or siblings have it.
Both relationships suggest that genes play a role in setting people up for diabetes. But something in the environment has to push those genes into action, and scientists aren’t sure what those triggers are. It’s also not clear which genes are involved.
“People spend their whole careers trying to understand this stuff,” Albright says.
If you learn you have diabetes, don’t despair. There’s plenty you can do to live a long and healthy life. Also, know you’re not alone.
Reed encourages all newly diagnosed kids to go to one of the nation’s many diabetes camps. It can be hugely reassuring, she says, to be surrounded by other kids who feel like you do.
“It’s really amazing,” Reed says. “It’s a very supportive and tolerating environment for kids who are often the only ones at their school with diabetes. At diabetes camp, everyone is going through it together.”
Going Deeper:







