Tackling the novel coronavirus calls for novel ideas
New projects take on supply shortages, explore new treatments and vaccines, and more

A patch with tiny needles could deliver a future COVID-19 vaccine. The patch would go on like a Band-Aid and release the vaccine into the skin to trigger an immune response.
University of Pittsburgh
Amy Barnard used to work as a biomedical engineer at a hospital in Green Bay, Wisc. Sometimes she would help fix medical equipment used for patients with infections. She often had to don a mask for this, along with gloves, booties, coveralls and more. Afterward, much of that personal protective equipment, or PPE, went right into the trash.
Then the COVID-19 pandemic hit.
Suddenly, thousands and thousands of people were getting sick from the contagious disease. Almost as suddenly, PPE supplies started to dry up.
“Hearing that they did not have enough was really tugging at my heart,” Amy says. Her current company, Therma-Tron-X, had already started to make face shields for a local hospital. She and her husband Daniel wanted to do more.
“Everyone is focusing on how to make PPE faster,” she thought. “What about the ability to reuse it more safely?” In late March, she sketched out an idea for a small sterilization unit. Her husband scaled up its size. Then he called his cousin Andrew. “Do you need a COVID idea?” he asked.
Andrew Barnard heads the Great Lakes Research Center at Michigan Technological University in Houghton. Normally a project like the sterilizer would take about a year to build, notes this mechanical engineer. But the COVID-19 pandemic motivated them to work fast. Really fast. People with different skills got involved. And that “really spurred innovation,” Andrew says.
The unit’s shell started out as a refrigerated truck container. It arrived in Houghton on March 31. A week later, the team had completed a working prototype. The system uses heat to sterilize items. Parts to build it can be found in most towns.
As some team members assembled the unit, Michigan Tech technical writers Lindsey Wells and Sidona DeBrule created a manual. It tells hospitals how to properly use the system. The challenge, Wells says, was figuring out how to describe that “when it’s not finished yet.”
Other researchers in Michigan are now running more tests. Some will confirm that process indeed kills the virus that causes COVID-19. Others will test what types of protective gear it can sterilize. Equally important: How many times can PPE be treated and still protect the people who wear it?
Welcome to the world of invention and innovation during a global pandemic. Groups around the world are stepping up to address equipment shortages caused by the spread of this new disease, such as PPE. Other teams hope to improve treatments for patients who’ve gotten sick. Still more researchers are racing to develop a vaccine that could quickly protect people.
Because COVID-19 is a novel disease, scientists and engineers are trying lots of new things. Yet their work includes approaches common to the process of invention. Some tweak existing ideas or systems. Others may turn to parts commonly found in stores but used for other purposes.

Protective gear
One new PPE sterilizer builds on a project that was already in the works. For several years, researchers at Battelle Memorial Institute in Columbus, Ohio, had been working on a system to wipe out killer germs. Their motivation: countering biological warfare — the unethical use of germs for the purpose of sickening people, plants or animals. The Battelle group now realized its tools and skills might also help fight a pandemic.
So-called N95 face masks have been designed to filter out bacteria and viruses from the air. These masks are the type preferred by medical staff who might attend to patients sick with COVID-19. But in the pandemic, some hospitals use more of these masks in a week than they used to need in three or more months. With these masks now in short supply, finding a way to reuse these single-use items suddenly became very appealing. But that gear would have to be cleaned. Otherwise, doctors, nurses and other staff would not be safe.
Battelle’s system turns a 35-percent solution of hydrogen peroxide into a vapor. Then it circulates this gas through a closed chamber holding the masks. Tiny droplets form. That’s called micro-condensation. “Think of the fog you see on your bathroom mirror when taking a shower,” explains Will Richter. He’s a microbiologist at Battelle.
Labs have used a similar setup to sterilize other things. “So it seemed like a logical choice, to us, to use for the N95 [mask] contamination,” Richter says. The original process had been designed to kill the spores of certain types of fungus. Within a week, his team had adapted that project for the virus that causes COVID-19. And those researchers have now confirmed that their process kills this virus.
Because of COVID-19, federal regulators on March 20 okayed the emergency use of this system. Within a few weeks, prototypes were at work in several cities. Each can sterilize 20,000 masks in a single load.
Other projects are adapting existing products and processes to deal with new problems. When the epidemic struck, supplies of alcohol-based hand sanitizer soon were exhausted.
Among places in great need was a major hospital and medical-research complex in Ohio known as the Cleveland Clinic. A nearby company, Cleveland Whiskey, took note. Alcohol “is what we make,” notes Tom Lix, who heads the whiskey distillery. And the firm already had an innovative process to make whiskey in a few months instead of years. It uses pressure changes to get liquid in steel containers to move in and out of oak or other wood chips in the mix. When the Cleveland Clinic put out a desperate call for hand sanitizer, Lix offered to help.
“We can make hand sanitizer with [our] alcohol,” he realized. Pharmacists from the hospital worked out a formula. Lix’s team then modified his production plant to make it. Its process now distills ethanol, a type of alcohol, to a higher concentration than is used in whiskey. A chemical called a denaturant (Dee-NAY-chur-unt) goes in to make the clear sanitizer taste awful. (The isopropyl alcohol sold in stores is poisonous.) Other ingredients include hydrogen peroxide and glycerin.
“Everything we make we give to the [Cleveland] Clinic,” Lix says. Other companies have now joined the effort, donating alcohol and supplies as well. Says Lix, “I think innovation is more about thinking differently and reacting to things differently.”

Speeding up contact tracing
Some COVID-driven innovations build on computing advances. One ongoing problem for contagious diseases is tracing with whom a sick person might have come into contact. Medical teams usually ask coronavirus patients to name everyone they met with in the previous two weeks. But this can be hard. Some of those contacts may have been strangers. They can include a store clerk or people someone talked to while walking the dog.
Ron Rivest is a computer scientist at the Massachusetts Institute of Technology in Cambridge. Before COVID-19 hit, he and others had invented computer programs to encrypt data. They came up with algorithms. These are directions for a computer program to follow. Rivest’s team has now used its computing skills to develop algorithms to track down those contacts.
The system uses data that’s already on most smartphones. “We were inspired by the Apple Find My system,” Rivest recalls. Bluetooth technology on smartphones routinely sends out signals, called chirps. Those chirps are received by any nearby Bluetooth device, such as another phone. So any phone with Bluetooth will have data about chirps it sent out and chirps it got from other smartphones it had been near.
In the system by Rivest’s team, a healthcare worker would ask a COVID-19 patient for access to that data. Information about the stored chirps would then become part of a large public database. People would check the database to see if they might have been exposed to someone with the virus. An app could do this automatically each day. If there had been a potential contact, someone could then stay away from others or get tested for the virus.
And the system can do all of this without giving away anyone’s names, phone numbers or locations. One catch: Only about half of U.S. adults might use the app. That figure comes from an April 2020 poll by the Washington Post and the University of Maryland.
New medicines and vaccines
COVID-19 currently has no known preventive medicines or cures. And that has spurred researchers the world over to find candidates. “There literally are hundreds of therapies” being tested, notes Derek Angus. He’s a critical care doctor at the University of Pittsburgh in Pennsylvania. What works best so far? “We don’t know,” he admits.
To help, he and others invented a tool that relies on artificial intelligence. As ongoing drug trials move ahead, this tool “learns” from data about all those trials. And it constantly updates itself. This can help doctors choose a treatment with the best chance of working, based on the latest data.
In a way, it’s testing many drugs and combinations at once, Angus explains. Other fields of medicine have used a similar approach. But this is the first time it’s been used for acute care of an urgent medical problem.
The idea for the tool began after a widespread H1N1 flu pandemic in 2009. “Everyone scrambled to do traditional clinical trials,” Angus says. Each trial needed hundreds of patients and could take months. However, he notes, “By the time they got up and running, H1N1 had left their region and gone somewhere else.” Angus and his colleagues think their approach will home in more quickly on potentially useful treatments.
Another group at his school is among dozens of teams now working to develop vaccines against COVID-19. That could keep people from getting the disease in the first place.
The Pittsburgh candidate got its start in research begun during the SARS epidemic in 2002 and 2003. Work back then showed how a coronavirus uses a “spike protein” to invade cells. Work with another coronavirus, which causes an illness called MERS, showed that a vaccine with bits of the spike protein could get the body to make antibodies. The Pittsburgh team is now using that approach.
Several research groups have been looking to deliver vaccines with a press-on patch. Louis Falo describes these as “Band-Aid-like.” A skin doctor at the University of Pittsburgh, he is working on one such device. Its teeny, tiny needles are made of a sugar-like substance. When pressed on, the patch’s needles pierce the skin and soon dissolve. This releases the vaccine.
Similar patch systems have been tried with measles and flu vaccines. One advantage to these is that they avoid the “ouch” of a big needle. Plus, vaccine delivered in this way needs no refrigeration. So shipping and storing it are easier, especially in low-income countries where refrigeration may be scarce.

‘We can do it’
Among other pandemic-inspired projects underway across the globe is a device from a team in Spain. It can scan people coming into an area to see if they have a fever. The trick: it uses a heat-sensing camera system.
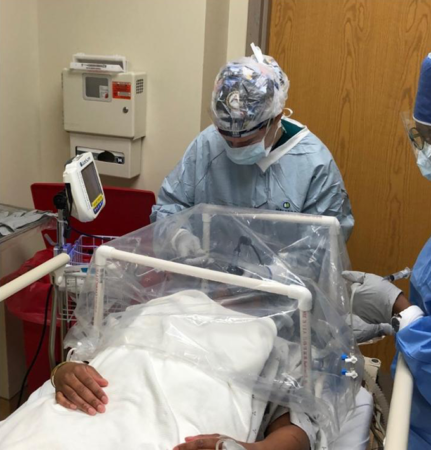
For another project, doctors working with the U.S. Department of Defense have invented a mini-isolation chamber for COVID-19 patients. This tent of plastic sheeting covers a patient’s head and shoulders. It allows medical staff to work more safely on or near the patient.
Face shields are one type of PPE in short supply. One team in Japan has now invented a do-it-yourself substitute. Medical doctor Kiyokazu Nakajima and others at the Osaka University Graduate School of Medicine brainstormed to come up with its design. Their fix relies on 3-D printing. It pairs a clear plastic file folder with a 3-D printed frame to hold it.
“This folder is available almost everywhere in the office,” Nakajima says. To get the frame to work, his group got help from Charmant. It’s a company that makes eyeglasses. Free instructions to make the masks are online, although you’ll need a 3-D printer to create the frame.
The COVID-19 pandemic is unlike anything that people alive today have ever encountered. Yet it likely won’t be the last global threat. The inventions and innovations underway now offer hope for dealing with the new pandemic — and perhaps those in the future.
There’s also a strong sense of determination and resilience. Remember the mobile sanitizing unit. That started with Amy Barnard talking at home with her husband. A whole crew then built the working prototype in just a few days.
“The biggest thing that I learned … is we can do it,” says Andrew Barnard in Michigan. “If there’s something else out there and it needs a tech solution, we can do it.”







